This site is intended for US healthcare professionals

NF1-PN can impact every aspect of patients’ lives
I don’t wear short shorts because of the PN on my thigh. I only wear longer shorts or pants.
– Lindsey, living with NF1-PN
Neurofibromatosis type 1 (NF1) is not rare in rare disease
- NF1 is more common than cystic fibrosis (estimated at 1 in 3000 to 6000 people worldwide) and muscular dystrophy (estimated at 1 in 3500 to 5000 people worldwide)1-3
- NF1 is the most prevalent of the known neurofibromatosis (NF) syndromes, a group of genetic disorders that are associated with the development of tumors on nerve tissues4
- Other neurofibromatosis syndromes include NF2-related schwannomatosis and schwannomatosis4,5
NF1-PN can be a complex disease to manage
- Plexiform neurofibromas (PNs) can grow anywhere on the body outside of the CNS; the most common location is the head and neck area, followed by the extremities and trunk6,7,*,†
- The growth rate of PNs is unpredictable, and there may be periods of rapid growth followed by periods of relative inactivity8-11
- Pediatric patients with NF1 and symptomatic PNs have a higher mortality rate compared to those without PNs or with asymptomatic PNs6,*
- Patients with NF1 have an 8% to 16% lifetime risk of transformation to malignant peripheral nerve sheath tumors (MPNSTs)12,13
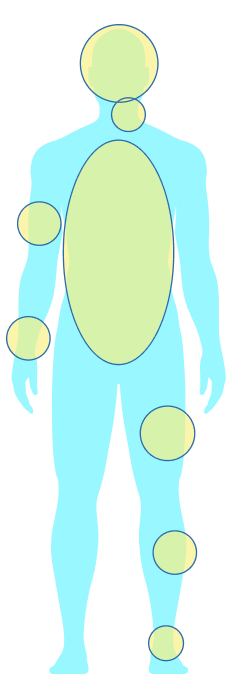
CNS=central nervous system.
Unresectable tumors, incomplete resections, and tumor regrowth limit the utility of surgical intervention14,15
- Debulking surgery may be considered for large PNs that are interfering with vital structures, including the airway or spinal cord, or for PNs that could lead to functional decline or changes in appearance14,16
- However, the feasibility of surgery can be restricted by tumor site or infiltration of surrounding nerves and vasculature17
- Even when surgery is feasible, complete removal of a plexiform neurofibroma (PN) is not possible in many cases6,18
- Rates of PN regrowth following incomplete resection have been reported to range from 29% to ~70% depending on the extent of resection6,17,*,‡
- In a survey, 16% (5/32) of patients with NF1-PN who received debulking surgery reported complications19,§
- Of the patients assessed for surgical complications associated with debulking surgery, 9% (3/32) experienced acute surgical complications, including delayed healing and bleeding, and 6% (2/32) experienced chronic postoperative symptoms, such as functional impairment and nerve damage
Up to ~85% of PNs
are not amenable to complete resection1,17,20
23% of PNs
regrow after a complete resection21,||
– Krista, living with NF1-PN
NF1 patients and caregivers may be coping with a substantial QoL burden7,22-32
Physical morbidities
- Pain
- Impaired mobility
- Changes in appearance
- Visual impairment
- Airway obstruction
- Spinal cord compression
- Tumors putting pressure on organs
Psychological impact
- Depression
- Anxiety
- Isolation
- Low self-esteem
- Stigma
- Embarrassment
- Fear of cancer
- Impaired sexual health
Cognitive deficits
- Inability to focus
- Impaired memory
- Impaired visual and motor function
- Learning disabilities
Logistical setbacks
- Trouble finding an HCP who specializes in NF
- Financial barriers/lack of insurance
- Travel barriers
- Difficulty coordinating appointments
In a survey about NF1-PN burden19,§:
PAIN
In a study of patients with NF1-PN7,†:
SAW CHANGES IN THEIR APPEARANCE
In a separate study of patients with
NF124,¶:
ANXIETY
(44/82)
DEPRESSION
(63/82)
“When I was younger, I wondered what people thought when they saw the PN on my leg because it’s visible when I’m wearing a bathing suit and it’s kind of embarrassing.”
– Lindsey, living with NF1-PN
HCP=healthcare provider; QoL=quality of life.
Many patients learn to live with their symptoms

I’m up 4 or 5 times at night because the pillow doesn’t feel right. I’ve just learned to accept it.
– Krista, living with NF1-PN


– Antwan, living with NF1-PN


– Lindsey, living with NF1-PN

NF1-PN can be challenging for young adults
For patients who are transitioning to adulthood, NF1-PN can be particularly burdensome.
‡
Based on a cross-sectional study using a one-time survey of NF1-PN patients and caregivers. Sixty-one pediatric patients 8 to 18 years old and their caregivers, and 21 additional caregivers of patients 2 to 7 years old (total of 82 caregivers) participated in the survey.19
||
Based on a retrospective analysis of clinical and MRI data of 52 children and adults with NF1 who had surgery to remove PNs at a referral center in Germany.21
¶
Based on a retrospective cohort study of 82 NF1 patients with a comorbid diagnosis of depression, anxiety, and/or attention-deficit hyperactivity disorder.24
Based on a qualitative study where clinicians (n=8), NF1-PN patients aged 5 years and older (n=31), and parents of NF1-PN patients aged 5 to 17 years (n=17) were interviewed to elicit the PN-related symptoms and concerns considered most important to assess.27
**
Based on SpringWorks Therapeutics–sponsored market research that included 4 adult NF1-PN patients and 11 NF1-PN caregivers. Both patients and caregivers were asked to identify the emotional and experiential impact of NF1-PN on patients.32
- Ejerskov C, Farholt S, Nielsen FSK, et al. Clinical characteristics and management of children and adults with neurofibromatosis type 1 and plexiform neurofibromas in Denmark: a nationwide study. Oncol Ther. 2023;11(1):97-110.
- Scotet V, L’Hostis C, Férec C. The changing epidemiology of cystic fibrosis: incidence, survival and impact of the CFTR gene discovery. Genes (Basel). 2020;11(6):589.
- Kariyawasam D, D’Silva A, Mowat D, et al. Incidence of Duchenne muscular dystrophy in the modern era; an Australian study. Eur J Hum Genet. 2022;30(12):1398-1404.
- Tamura R. Current understanding of neurofibromatosis type 1, 2, and schwannomatosis. Int J Mol Sci. 2021;22(11):5850.
- Plotkin SR, Messiaen L, Legius E, et al. Updated diagnostic criteria and nomenclature for neurofibromatosis type 2 and schwannomatosis: an international consensus recommendation. Genet Med. 2022;24(9):1967-1977.
- Prada CE, Rangwala FA, Martin LJ, et al. Pediatric plexiform neurofibromas: impact on morbidity and mortality in neurofibromatosis type 1. J Pediatr. 2012;160(3):461-467.
- Darrigo LG Jr, Ferraz VEF, Cormedi MCV, et al. Epidemiological profile and clinical characteristics of 491 Brazilian patients with neurofibromatosis type 1. Brain Behav. 2022;12(6):e2599.
- Ferner RE, Huson SM, Thomas N, et al. Guidelines for the diagnosis and management of individuals with neurofibromatosis 1. J Med Genet. 2007;44(2):81-88.
- Akshintala S, Baldwin A, Liewehr DJ, et al. Longitudinal evaluation of peripheral nerve sheath tumors in neurofibromatosis type 1: growth analysis of plexiform neurofibromas and distinct nodular lesions. Neuro Oncol. 2020;22(9):1368-1378.
- Ly KI, Merker VL, Cai W, et al. Ten-year follow-up of internal neurofibroma growth behavior in adult patients with neurofibromatosis type 1 using whole-body MRI. Neurology. 2023;100(7):e661-e670.
- Nguyen R, Dombi E, Widemann BC, et al. Growth dynamics of plexiform neurofibromas: a retrospective cohort study of 201 patients with neurofibromatosis 1. Orphanet J Rare Dis. 2012:7:75.
- Higham CS, Dombi E, Rogiers A, et al. The characteristics of 76 atypical neurofibromas as precursors to neurofibromatosis 1 associated malignant peripheral nerve sheath tumors. Neuro Oncol. 2018;20(6):818-825.
- Miettinen MM, Antonescu CR, Fletcher CDM, et al. Histopathologic evaluation of atypical neurofibromatous tumors and their transformation into malignant peripheral nerve sheath tumor in patients with neurofibromatosis 1—a consensus overview. Hum Pathol. 2017;67:1-10.
- Fisher MJ, Blakeley JO, Weiss BD, et al. Management of neurofibromatosis type 1-associated plexiform neurofibromas. Neuro Oncol. 2022;24(11):1827-1844.
- Metrock LK, Lobbous M, Korf B. An evaluation of selumetinib for the treatment of neurofibromatosis type 1-associated symptomatic, inoperable plexiform neurofibromas. Expert Rev Precis Med Drug Dev. 2021;6(4):239-246.
- Armstrong AE, Belzberg AJ, Crawford JR, Hirbe AC, Wang ZJ. Treatment decisions and the use of MEK inhibitors for children with neurofibromatosis type 1-related plexiform neurofibromas. BMC Cancer. 2023;23(1):553.
- Needle MN, Cnaan A, Dattilo J, et al. Prognostic signs in the surgical management of plexiform neurofibroma: the Children’s Hospital of Philadelphia experience, 1974-1994. J Pediatr. 1997;131(5):678-682.
- Yang X, Desai K, Agrawal N, et al. Treatment, resource use and costs among pediatric patients with neurofibromatosis type 1 and plexiform neurofibromas. Pediatric Health Med Ther. 2020;11:421-428.
- Yang X, Yoo HK, Amin S, et al. Clinical and humanistic burden among pediatric patients with neurofibromatosis type 1 and plexiform neurofibroma in the USA. Childs Nerv Syst. 2022;38(8):1513-1522.
- Wolkenstein P, Chaix Y, Entz Werle N, et al. French cohort of children and adolescents with neurofibromatosis type 1 and symptomatic inoperable plexiform neurofibromas: CASSIOPEA study. Eur J Med Genet. 2023;66(5):104734.
- Nguyen R, Ibrahim C, Friedrich RE, Westphal M, Schuhmann M, Mautner V-F. Growth behavior of plexiform neurofibromas after surgery. Genet Med. 2013;15(9):691-697.
- Gross AM, Singh G, Akshintala S, et al. Association of plexiform neurofibroma volume changes and development of clinical morbidities in neurofibromatosis 1. Neuro Oncol. 2018;20(12):1643-1651.
- Miller DT, Freedenberg D, Schorry E, Ullrich NJ, Viskochil D, Korf BR; Council on Genetics; American College of Medical Genetics and Genomics. Health supervision for children with neurofibromatosis type 1. Pediatrics. 2019;143(5):e20190660.
- Houpt AC, Schwartz SE, Coover RA. Assessing psychiatric comorbidity and pharmacologic treatment patterns among patients with neurofibromatosis type 1. Cureus. 2021;13(12):e20244.
- Foji S, Mohammadi E, Sanagoo A, Jouybari L. How do people with neurofibromatosis type 1 (the forgotten victims) live? a grounded theory study. Health Expect. 2022;25(2):659-666.
- Rosnau K, Hashmi SS, Northrup H, Slopis J, Noblin S, Ashfaq M. Knowledge and self-esteem of individuals with neurofibromatosis type 1 (NF1). J Genet Couns. 2017;26(3):620-627.
- Lai J-S, Jensen SE, Patel ZS, Listernick R, Charrow J. Using a qualitative approach to conceptualize concerns of patients with neurofibromatosis type 1 associated plexiform neurofibromas (pNF) across the lifespan. Am J Med Genet A. 2017;173(1):79-87.
- Fournier H, Calcagni N, Morice-Picard F, Quintard B. Psychosocial implications of rare genetic skin diseases affecting appearance on daily life experiences, emotional state, self-perception and quality of life in adults: a systematic review. Orphanet J Rare Dis. 2023;18(1):39.
- Radtke HB, Berger A, Skelton T, Goetsch Weisman A. Neurofibromatosis type 1 (NF1): addressing the transition from pediatric to adult care. Pediatric Health Med Ther. 2023;14:19-32.
- Leidger A, Vosschulte M, Nieder TO, Mautner V-F. Sexual self-esteem and psychological burden of adults with neurofibromatosis type 1. Front Psychol. 2022:13:883019.
- Crow AJD, Janssen JM, Marshall C, et al. A systematic review and meta-analysis of intellectual, neuropsychological, and psychoeducational functioning in neurofibromatosis type 1. Am J Med Genet A. 2022;188(8):2277-2292.
- Data on file: SpringWorks Therapeutics, Inc.
- Stewart DR, Korf BR, Nathanson KL, Stevenson DA, Yohay K. Care of adults with neurofibromatosis type 1: a clinical practice resource of the American College of Medical Genetics and Genomics (ACMG). Genet Med. 2018;20(7):671-682.
- Rietman AB, van Helden H, Both PH, et al. Worries and needs of adults and parents of adults with neurofibromatosis type 1. Am J Med Genet A. 2018;176(5):1150-1160.
- Oates EC, Payne JM, Foster SL, Clarke NF, North KN. Young Australian adults with NF1 have poor access to health care, high complication rates, and limited disease knowledge. Am J Med Genet A. 2013;161A(4):659-666.